

The heel is a highly specialized part of the body designed to absorb the shock of walking and running. When walking the stresses placed on your feet can be 11/4 times your body weight and, during your lifetime, you could walk the equivalent of four times around the world. These stresses can increase to 23/4 times body weight when running. It is therefore not surprising that heel pain is a common occurrence.
Although most heel pain tends to be caused by mechanical injury, as a result of small but repetitive injuries that occur at a rate faster than the body can heal them. There are times when it can be caused by injuries to the lower back or diseases such as inflammatory joint conditions.
If you experience heel pain, you could follow the simple self-care shown later. However, if the pain persists longer than 3 weeks and it is affecting you, it may be appropriate to seek professional advice. This is necessary, as there are many types of heel pain, each with different causes and sometimes requiring quite different forms of treatment.
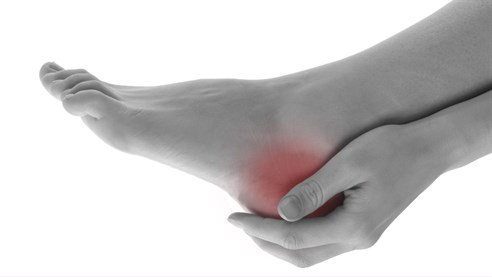
The following are some of the more common types of heel pain. This list, however, is not exhaustive, but may help you appreciate the complexity of heel pain and why specialist advice can be helpful.
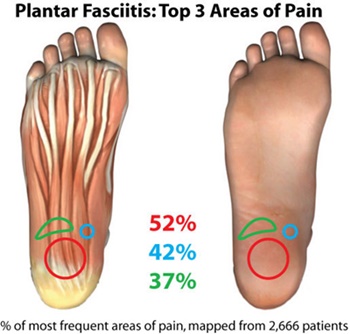
Probably the most common cause of pain in the heel results from damage to the tissue band (fascia) connecting the heel bone to the base of the toes. It tends to be painful when you take your first steps after resting and especially when getting out of bed in the morning. Most often associated with middle age, however, it can occur in all ages. Treatment will involve special stretching exercises and, if appropriate, shoe inserts designed to alter foot function which will reduce the tension within (and thereby injury to) the plantar fascia. Soft heel cushions rarely help the plantar fasciitis. Unfortunately, it can be a difficult condition to treat and sometimes it may be necessary to also consider medication.
This sometimes feels like a burning sensation and at other times a tingling sensation underneath the heel and in the arch of the foot. Occasionally there can be loss of sensation on the bottom of the foot. It is caused by compression of the tibial nerve as it passes the inside of the ankle and tapping of the nerve will stimulate the symptoms known as Tinel’s sign. Special shoe inserts can reduce the pressures on the nerve and may be appropriate for certain foot types. On other occasions local injections of medication to the area where the tibial nerve is inflamed may be necessary.
An inflammation of a bursa (a fluid filled fibrous sac) under the heel bone. Typically the pain is more to the centre of the heel than that which is experienced with plantar fasciitis and significantly it worsens during the day. Medication and ultrasound can give relief, but for long-term relief a shoe insert may be necessary.
Caused by a heavy heel strike or sometimes a reduction in the thickness of the heel pad, this can give rise to a dull ache in the heel when standing and walking that increases during the day. A soft heel cushion can help.
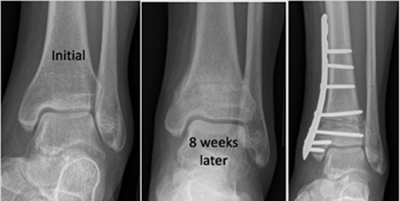
Can occur following injury, for example falling from a height. If this is suspected an X-ray would be required to confirm diagnosis and determine the extent of the injury
This condition affects young children, normally between the ages of 8 and 12. It occurs when part of the heel bone suffers a temporary loss of blood supply, and as a result the bone dies only to reform when the blood supply is later restored. It is a condition known as osteochondrosis that can occur in growing bones, and one that fortunately is self-limiting, but can be painful at the time.
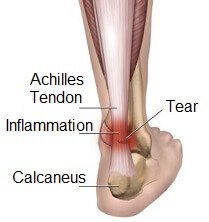
This can occur where the Achilles tendon is placed under more tension than it is able to cope with and so as a result small tears develop. These then become a source of further injury and gradually a swelling may develop within the tendon - this is called Achilles tendonosis (sometimes inappropriately referred to as tendonitis). Treatment will involve special;exercises that strengthen the tendon and temporarily increasing the height of the heel with an insole. Other forms of pain associated with the Achilles tendon include paratendonitis (involving tissues surrounding the tendon) and Achilles enthesis (inflammation of the insertion of the tendon to the heel). Once again differentiating between these conditions is important,as each requires slightly different treatments.
You can reduce the risk of heel pain in many ways, including:
Lose weight. Your body weight is magnified 2-4 times at the foot and ankle when walking. The loss of five pounds can reduce the force on your plantar fascia by up to 20 pounds with every step! This goes along way in the treatment of your injury.